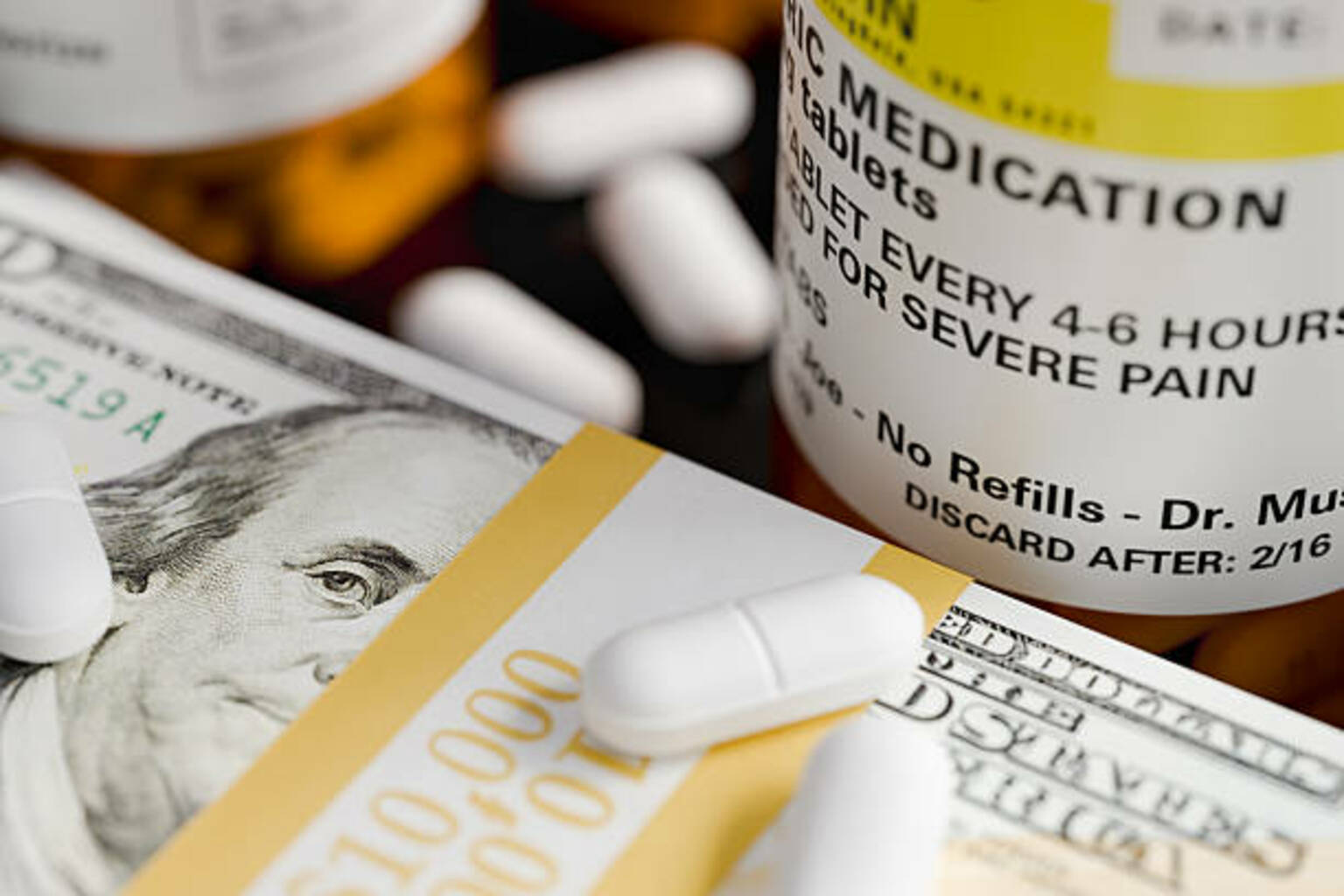
UnitedHealth Group Launches New Pharmacy Care Model
UnitedHealth Group's stock rose 3.01% and reached a 20-day high amid a challenging market, with the Nasdaq-100 down 1.48% and the S&P 500 down 0.41%.
The catalyst for this price movement is the announcement from UnitedHealth's pharmacy benefits division, Optum Rx, which introduced a new pharmacy care model that will charge clients a per-member monthly fee starting in 2027. This model aims to enhance transparency and affordability in pharmacy care, addressing criticisms regarding rising drug prices. Additionally, UnitedHealth plans to pass through all negotiated rebate discounts to clients by January 1, 2028, further strengthening its competitive position in the market.
This new pricing model is expected to improve client satisfaction and could lead to increased market share for UnitedHealth. The positive reception of this initiative may attract more investors, especially as the company continues to address transparency issues in the healthcare sector.
Trade with 70% Backtested Accuracy
Analyst Views on UNH
About UNH
About the author

- Significant Stock Fluctuation: UnitedHealth Group's stock price dropped from $336 to $259 at the beginning of 2023, but rebounded by over 47% to around $381 by May 11, indicating a gradual recovery after volatility.
- Q1 Performance Improvement: In Q1 2023, UnitedHealth's revenue increased by 2% year-over-year to $111.7 billion, with earnings per share exceeding expectations at $6.90 and adjusted EPS at $7.23, suggesting a turnaround after leadership upheaval and rising costs.
- Impact of Medicare Advantage: While Medicare Advantage provides revenue, payment rates have not kept pace with rising costs, leading UnitedHealth to cut 1.3 million members in 2026 to improve margins and ensure long-term sustainability.
- Investor Confidence Restoration: Despite facing regulatory challenges like an antitrust investigation, UnitedHealth's dividend yield of approximately 2.3% attracts long-term investors, making the current stock price appealing for buying or holding.
- New Pricing Model: UnitedHealth's pharmacy benefits division, Optum Rx, has introduced a new pharmacy care model that will charge clients a per-member monthly fee, set to launch in 2027, aimed at addressing transparency issues and eliminating spread pricing in traditional PBM models.
- Enhanced Transparency: This new model will bring greater clarity to Optum Rx's fees, including charges from its group purchasing organization, designed to fully align incentives with patients and plan sponsors, thereby improving predictability and affordability in pharmacy care.
- Addressing Drug Price Criticism: The pricing structure builds on several initiatives by Optum Rx to enhance affordability across the U.S. healthcare system, particularly in response to criticism regarding its role in rising U.S. drug prices.
- Future Plans: UnitedHealth plans to pass through all rebate discounts negotiated with drugmakers to clients by January 1, 2028, following an agreement made in January 2025, further strengthening its competitive position in the pharmacy care market.
- Legal Challenges: Optum Rx CEO John Mahrt highlighted that lawsuits from brand manufacturers are hindering the adoption of biosimilars, despite the company's desire to offer more options, with approximately 60% of customers insured by UnitedHealth.
- Transparent Pricing Model: On May 11, Optum Rx announced a transparent fee-based model where clients will pay clearly defined monthly fees per member, independent of manufacturers' list prices or prescription volumes, aiming to eliminate spread pricing and similar practices.
- Cost Reduction Initiatives: Mahrt emphasized that Optum is helping to lower medication costs by passing through 100% of drug rebates to plan sponsors and focusing on point-of-sale rebates to enhance economic benefits for clients.
- Support for Policy Reforms: Mahrt expressed support for reforms pushed by the Trump administration and some members of Congress regarding PBM influence, with relevant reforms included in the Consolidated Appropriations Act of 2026, aimed at ensuring 100% rebate pass-throughs and fixed-fee compensation.
- Tech-Driven Rebound: The Dow Jones Industrial Average has climbed back to 50,000 for the first time since February 10, primarily driven by stocks linked to artificial intelligence, highlighting the tech sector's dominant role in the economic recovery.
- Amazon's AI Strategy: Amazon's stock has surged 31% since February, as the company enhances its AI offerings by making Alexa the centerpiece of its shopping strategy, which is expected to drive future sales growth.
- UnitedHealth's Strong Performance: UnitedHealth's stock has skyrocketed 47% during the same period, bolstered by strong earnings and solid guidance from management, making it a key contributor to the Dow's return to 50,000, showcasing the resilience of the healthcare sector.
- Mixed Performance Among Stocks: Despite the Dow's rebound, most component stocks have underperformed, indicating a reliance on AI-driven growth, raising questions about the sustainability of the index's rise without support from other stocks.
- Goldman Sachs Confidence: Goldman Sachs added UnitedHealth Group to its U.S. conviction list, believing that its performance in the Medicare Advantage market is approaching an inflection point, which is expected to drive profit improvement and reflects strong bullish sentiment towards the stock.
- Medicare Advantage Strength: As of March 2026, UnitedHealth serves over 7.5 million Medicare Advantage members, and despite stock volatility over the past 18 months, Goldman Sachs believes the company is nearing the bottom of its underwriting cycle, with potential for future profit growth.
- Positive Market Response: Goldman Sachs' 12-month price target indicates an upside potential of about 12%, and among 28 analysts, 22 rated the stock as a
- Strong Q1 Performance: Major U.S. health insurers, including UnitedHealth Group and Cigna, reported first-quarter results exceeding analysts' expectations, indicating improved cost management capabilities despite industry pressures that have seen the S&P managed care index drop over 12% since July 2023.
- Stabilizing Medical Costs: Analysts noted that while medical costs have continued to rise in government-sponsored health plans, recent performances suggest that cost trends may be stabilizing, with potential for further positive earnings estimate revisions reflecting improving fundamentals in the industry.
- Upcoming Quarter Challenges: Analysts caution that the second quarter typically serves as a test for health insurers, with historical data indicating that claims may surprise in May, prompting investors to closely monitor the upcoming months for financial performance.
- Positive Market Reaction: Despite seasonal factors impacting costs, analysts maintain an optimistic view on the industry's core strength, suggesting that the improvement in medical costs may be sustainable rather than a temporary occurrence, indicating a gradual enhancement of the industry's fundamentals.